Memantine Hydrochloride Torrent 10 Mg/Ml Oral Solution
SUMMARY OF PRODUCT CHARACTERISTICS
1 NAME OF THE MEDICINAL PRODUCT
Memantine hydrochloride Torrent 10mg/ml oral solution
2 QUALITATIVE AND QUANTITATIVE COMPOSITION
Pump: Each actuation of the pump (one downward pump) delivers 0.5 ml of solution containing 5 mg of memantine hydrochloride equivalent to 4.16 mg of memantine.
Dosing Pipette: 0.5 ml contains 5 mg of memantine hydrochloride equivalent to 4.16 mg of memantine.
Each millilitre of solution contains 10mg of memantine hydrochloride.
Excipients with known effect:
Each millilitre of solution contains 100 mg sorbitol (E420) and 0.5mg of potassium, see section 4.4.
For the full list of excipients, see section 6.1.
3 PHARMACEUTICAL FORM
Oral Solution.
The solution is clear to colourless to light yellowish
4 CLINICAL PARTICULARS
4.1 Therapeutic indications
Treatment of patients with moderate to severe Alzheimer’s disease.
4.2 Posology and method of administration
Treatment should be initiated and supervised by a physician experienced in the diagnosis and treatment of Alzheimer's dementia. Therapy should only be started if a caregiver is available who will regularly monitor the intake of the medicinal product by the patient. Diagnosis should be made according to current guidelines The tolerance and dosing of memantine should be reassessed on a regular basis, preferably within three months after start of treatment. Thereafter, the clinical benefit of memantine and the patient’s tolerance of treatment should be reassessed on a regular basis according to current clinical guidelines. Maintenance treatment can be continued for as long as a therapeutic benefit is favourable and the patient tolerates treatment with memantine. Discontinuation of memantine should be considered when evidence of a therapeutic effect is no longer present or if the patient does not tolerate treatment..
This medicinal product should be taken once daily at the same time each day. The solution must not be poured, pumped or pipetted into the mouth directly from the bottlepump or pipette, but should be dosed onto a spoon or into a glass of water using the pump or pipette.
For detailed instructions on the preparation and handling of the product see section 6.6.
The solution can be taken with or without food.
Adults:
Dose titration
The maximum daily dose is 20 mg daily. In order to reduce the risk of undesirable effects the maintenance dose is achieved by upward titration of 5 mg per week over the first 3 weeks as follows: (a)Pump pack of 5 mg/pump:
Week I (day 1 “ 7):
The patient should take 0.5 ml solution (5 mg) equivalent to one downward pump, per day for 7 days.
Week 2 (day 8 _ 14):
The patient should take 1 ml solution (10 mg) equivalent to two downward pumps, per day for 7 days.
Week 3 (day 15-21):
The patient should take 1.5 ml solution (15 mg) equivalent to three downward pumps per day for 7 days.
From Week 4 on:
The patient should take 2 ml solution (20 mg) equivalent to four downward pumps, once a day.
(b) Dosing Pipette:
Week 1 (day 1 “ 7):
The patient should take 0.5 ml solution (5 mg) for 7 days.
Week 2 (day 8 - 14):
The patient should take 1 ml solution (10 mg) for 7 days.
Week 3 (day 15-21):
The patient should take 1.5 ml solution (15 mg) for 7 days.
From Week 4 on:
The patient should take 2 ml solution (20 mg) once a day.
Maintenance Dose
The recommended maintenance dose is 20 mg per day.
Elderly: On the basis of the clinical studies, the recommended dose for patients over the age of 65 years is 20 mg per day (2 ml solution, equivalent to four downward pumps) as described above.
Children and adolescents under the age of 18 years: This medicinal product is not recommended for use in children below 18 years due to a lack of data on safety and efficacy.
Renal impairment: In patients with mildly impaired renal function (creatinine clearance 50 - 80 ml/min) no dosage adjustment is required. In patients with moderate renal impairment (creatinine clearance 30 - 49 ml/min) daily dose should be 10 mg (1 ml solution, equivalent to two downward pumps). If tolerated well after at least 7 days of treatment, the dose could be increased up to 20 mg/day according to standard titration scheme. In patients with severe renal impairment (creatinine clearance 5 - 29 ml/min) daily dose should be 10 mg (1 ml solution, equivalent to two downward pumps) per day.
Hepatic impairment: In patients with mild or moderate hepatic impaired function (Child-Pugh A and Child-Pugh B) no dosage adjustment is needed. No data on the use of memantine in patients with severe hepatic impairment are available. Administration of this medicinal product is not recommended in patients with severe hepatic impairment.
4.3 Contraindications
Hypersensitivity to the active substance or to any of the excipients listed in 6.1.
4.4 Special warnings and precautions for use
Caution is recommended in patients with epilepsy, former history of convulsions or patients with predisposing factors for epilepsy.
Concomitant use of N-methyl-D-aspartate (NMDA)-antagonists such as amantadine, ketamine or dextromethorphan should be avoided. These compounds act at the same receptor system as memantine, and therefore adverse drug reactions (mainly central nervous system (CNS)-related) may be more frequent or more pronounced (see also section 4.5).
Some factors that may raise urine pH (see section 5.2 “Elimination”) may necessitate careful monitoring of the patient. These factors include drastic changes in diet, e.g. from a carnivore to a vegetarian diet, or a massive ingestion of alkalising gastric buffers. Also, urine pH may be elevated by states of renal tubulary acidosis (RTA) or severe infections of the urinary tract with Proteus bacteria.
In most clinical trials, patients with recent myocardial infarction, uncompensated congestive heart failure (NYHA III-IV), or uncontrolled hypertension were excluded. As a consequence, only limited data are available and patients with these conditions should be closely supervised.
Excipients: The oral solution contains sorbitol. Patients with rare hereditary problems of fructose intolerance should not take this medicine.
4.5 Interaction with other medicinal products and other forms of interaction
Due to the pharmacological effects and the mechanism of action of memantine the following interactions may occur.
• The mode of action suggests that the effects of L-dopa, dopaminergic agonists, and anticholinergics may be enhanced by concomitant treatment with NMDA-antagonists such as memantine. The effects of barbiturates and neuroleptics may be reduced. Concomitant administration of memantine with the antispasmodic agents, dantrolene or baclofen, can modify their effects and a dosage adjustment may be necessary.
• Concomitant use of memantine and amantadine should be avoided, owing to the risk of pharmacotoxic psychosis. Both compounds are chemically related NMDA-antagonists. The same may be true for ketamine and dextromethorphan (see also section 4.4). There is one published case report on a possible risk also for the combination of memantine and phenytoin.
• Other active substances such as cimetidine, ranitidine, procainamide, quinidine, quinine and nicotine that use the same renal cationic transport system as amantadine may also possibly interact with memantine leading to a potential risk of increased plasma levels.
• There may be a possibility of reduced serum level of hydrochlorothiazide (HCT) when memantine is co-administered with HCT or any combination with HCT.
• In post-marketing experience, isolated cases with international normalized ratio (INR) increases have been reported in patients concomitantly treated with warfarin. Although no causal relationship has been established, close monitoring of prothrombin time or INR is advisable for patients concomitantly treated with oral anticoagulants.
In single dose pharmacokinetic (PK) studies in young healthy subjects, no relevant active substance-active substance interaction of memantine with glyburide/metformin or donepezil was observed.
In a clinical study in young healthy subjects, no relevant effect of memantine on the pharmacokinetics of galantamine was observed.
Memantine did not inhibit CYP 1A2, 2A6, 2C9, 2D6, 2E1, 3A, flavin-containing monooxygenase, epoxide hydrolase or sulphation in vitro.
4.6 Fertility, pregnancy and lactation
Pregnancy:
For memantine, no clinical data on exposed pregnancies are available. Animal studies indicate a potential for reducing intrauterine growth at exposure levels, which are identical or slightly higher than at human exposure (see section 5.3). The potential risk for humans is unknown. Memantine should not be used during pregnancy unless clearly necessary.
Breast Feeding:
It is not known whether memantine is excreted in human breast milk but, taking into consideration the lipophilicity of the substance, this probably occurs. Women taking memantine should not breast-feed.
4.7 Effects on ability to drive and use machines
Moderate to severe Alzeimer’s disease usually causes impairment of driving performance and compromises the ability to use machinery. Furthermore, this medicinal product has minor or moderate influence on the ability to drive or use machines, such that outpatients should take special care.
4.8 Undesirable effects
In clinical trials in mild to severe dementia, involving 1,784 patients treated with this memantine hydrochloride and 1,595 patients treated with placebo, the overall incidence rate of adverse reactions with this memantine hydrochloride did not differ from those with placebo; the adverse events were usually mild to moderate in severity. The most frequently occurring adverse reactions with a higher incidence in this medicinal product group than in the placebo group were dizziness (6.3% vs 5.6%, respectively), headache (5.2% vs 3.9%), constipation (4.6% vs 2.6%), somnolence (3.4% vs 2.2%) and hypertension (4.1% vs 2.8%).
The following Adverse Drug Reactions listed in the Table below have been accumulated in clinical studies with this memantine hydrochloride and since its introduction in the market. Within each frequency grouping, undesirable effects are presented in order of decreasing seriousness.
Adverse reactions are ranked according to system organ class, using the following convention: very common ( ^ 1/10), common ( ^ 1/100 to < 1/10), uncommon ( ^ 1/1,000 to < 1/100), rare ( £ 1/10,000 to < 1/1,000), very rare (< 1/10,000), not known (cannot be estimated from the available data).
|
System organ class |
Frequency |
Undesirable Effect |
|
Infections and infestations |
Uncommon |
Fungal Infections |
|
Immune system disorders |
Common |
Drug Hypersensitivity |
|
Psychiatric disorders |
Common |
Somnolence |
|
Uncommon |
Confusion | |
|
Uncommon |
Hallucinations1 | |
|
Not known |
Psychotic reactions2 | |
|
Nervous system disorders |
Common |
Dizziness |
|
Uncommon |
Balance disorders | |
|
Very Rare |
Seizures | |
|
Cardiac disorders |
Uncommon |
Cardiac Failure |
|
Vascular disorders |
Common |
Hypertension |
|
Uncommon |
Venous thrombosis/thromboembolism | |
|
Respiratory, thoracic and mediastinal disorders |
Common |
Dyspnoea |
|
Gastrointestinal disorders |
Common |
Constipation |
|
Uncommon |
Vomiting | |
|
Not known |
Pancreatitis2 |
|
Hepatobiliary disorders |
Common |
Elevated Liver Function Test |
|
Not known |
Hepatitis | |
|
General disorders and administration site conditions |
Common |
Headache |
|
Uncommon |
Fatigue |
1 Hallucinations have mainly been observed in patients with severe Alzheimer's disease.
2 Isolated cases reported in post-marketing experience.
Alzheimer's disease has been associated with depression, suicidal ideation and suicide. In post-marketing experience these events have been reported in patients treated with this medicinal product.
Reporting of suspected adverse reactions
Reporting suspected adverse reactions after authorisation of the medicinal product is important. It allows continued monitoring of the benefit/risk balance of the medicinal product.
Healthcare professionals are asked to report any suspected adverse reactions via the Yellow Card Scheme at: www.mhra.gov.uk/yellowcard.
4.9 Overdose
Only limited experience with overdose is available from clinical studies and postmarketing experience.
Symptoms: Relatively large overdoses (200 mg and 105 mg/day for 3 days, respectively) have been associated with either only symptoms of tiredness, weakness and/or diarrhoea or no symptoms. In the overdose cases below 140 mg or unknown dose the patients revealed symptoms from central nervous system (confusion, drowsiness, somnolence, vertigo, agitation, aggression, hallucination, and gait disturbance) and/or of gastrointestinal origin (vomiting and diarrhoea).
In the most extreme case of overdose, the patient survived the oral intake of a total of 2000 mg memantine with effects on the central nervous system (coma for 10 days, and later diplopia and agitation). The patient received symptomatic treatment and plasmapheresis. The patient recovered without permanent sequelae.
In another case of a large overdose, the patient also survived and recovered. The patient had received 400 mg memantine orally. The patient experienced central nervous system symptoms such as restlessness, psychosis, visual hallucinations, proconvulsiveness, somnolence, stupor, and unconsciousness.
Treatment: In the event of overdose, treatment should be symptomatic. No specific antidote for intoxication or overdose is available. Standard clinical procedures to remove active substance material, e.g. gastric lavage, carbo medicinalis (interruption of potential entero-hepatic recirculation), acidification of urine, forced diuresis should be used as appropriate.
In case of signs and symptoms of general central nervous system (CNS) overstimulation, careful symptomatic clinical treatment should be considered.
5 PHARMACOLOGICAL PROPERTIES
5.1 Pharmacodynamic properties
Pharmacotherapeutic group: Anti-dementia drugs, ATC code: N06DX01.
There is increasing evidence that malfunctioning of glutamatergic neurotransmission, in particular at NMDA-receptors, contributes to both expression of symptoms and disease progression in neurodegenerative dementia.
Memantine is a voltage-dependent, moderate-affinity uncompetitive NMDA-receptor antagonist. It modulates the effects of pathologically elevated tonic levels of glutamate that may lead to neuronal dysfunction.
Clinical studies: A pivotal monotherapy study in a population of patients suffering from moderate to severe Alzheimer's disease (mini mental state examination (MMSE) total scores at baseline of 3 -14) included a total of 252 outpatients. The study showed beneficial effects of memantine treatment in comparison to placebo at 6 months (observed cases analysis for the clinician's interview based impression of change (CIBIC-plus): p=0.025; Alzheimer's disease cooperative study - activities of daily living (ADCS-ADLsev): p=0.003; severe impairment battery (SIB): p=0.002)
A pivotal monotherapy study of memantine in the treatment of mild to moderate Alzheimer's disease (MMSE total scores at baseline of 10 to 22) included 403 patients. Memantine-treated patients showed a statistically significantly better effect than placebo-treated patients on the primary endpoints: Alzheimer's disease assessment scale (ADAS-cog) (p=0.003) and CIBIC-plus (p=0.004) at week 24 (last observation carried forward (LOCF)). In another monotherapy study in mild to moderate Alzheimer's disease a total of 470 patients (MMSE total scores at baseline of 11-23) were randomised. In the prospectively defined primary analysis statistical significance was not reached at the primary efficacy endpoint at week 24.
A meta-analysis of patients with moderate to severe Alzheimer's disease (MMSE total scores < 20) from the six phase III, placebo-controlled, 6 - month studies (including monotherapy studies and studies with patients on a stable dose of acetylcholinesterase inhibitors) showed that there was a statistically significant effect in favour of memantine treatment for the cognitive, global, and functional domains. When patients were identified with concurrent worsening in all three domains, results showed a statistically significant effect of memantine in preventing worsening, as twice as many placebo-treated patients as memantine-treated patients showed worsening in all three domains (21% vs. 11%, p<0.0001).
5.2 Pharmacokinetic properties
Absorption: Memantine has an absolute bioavailability of approximately 100%. tmax is between 3 and 8 hours. There is no indication that food influences the absorption of memantine.
Distribution: Daily doses of 20 mg lead to steady-state plasma concentrations of memantine ranging from 70 to 150 ng/ml (0.5 - 1 pmol) with large interindividual variations. When daily doses of 5 to 30 mg were administered, a mean cerebrospinal fluid (CSF)/serum ratio of 0.52 was calculated. The volume of distribution is around 10 l/kg. About 45% of memantine is bound to plasma-proteins.
Biotransformation: In man, about 80% of the circulating memantine-related material is present as the parent compound. Main human metabolites are N-3,5-dimethyl-gludantan, the isomeric mixture of 4- and 6-hydroxy-memantine, and 1-nitroso-3,5-dimethyl-adamantane. None of these metabolites exhibit NMDA-antagonistic activity. No cytochrome P 450 catalysed metabolism has been detected in vitro.
In a study using orally administered 14C-memantine, a mean of 84% of the dose was recovered within 20 days, more than 99% being excreted renally.
Elimination: Memantine is eliminated in a monoexponential manner with a terminal t/ of 60 to 100 hours. In volunteers with normal kidney function, total clearance (Cltot) amounts to 170 ml/min/1.73 m2 and part of total renal clearance is achieved by tubular secretion.
Renal handling also involves tubular reabsorption, probably mediated by cation transport proteins. The renal elimination rate of memantine under alkaline urine conditions may be reduced by a factor of 7 to 9 (see section 4.4). Alkalisation of urine may result from drastic changes in diet, e.g. from a carnivore to a vegetarian diet, or from the massive ingestion of alkalising gastric buffers.
Linearity: Studies in volunteers have demonstrated linear pharmacokinetics in the dose range of 10 to 40 mg.
Pharmacokinetic/pharmacodynamic relationship: At a dose of memantine of 20 mg per day the cerebrospinal fluid (CSF) levels match the ki-value (ki = inhibition constant) of memantine, which is 0.5 pmol in human frontal cortex.
5.3 Preclinical safety data
In short term studies in rats memantine like other NMDA-antagonists have induced neuronal vacuolisation and necrosis (Olney lesions) only after doses leading to very high peak serum concentrations. Ataxia and other preclinical signs have preceded the vacuolisation and necrosis. As the effects have neither been observed in long term studies in rodents nor in non-rodents, the clinical relevance of these findings is unknown.
Ocular changes were inconsistently observed in repeat dose toxicity studies in rodents and dogs, but not in monkeys. Specific ophthalmoscopic examinations in clinical studies with memantine did not disclose any ocular changes.
Phospholipidosis in pulmonary macrophages due to accumulation of memantine in lysosomes was observed in rodents. This effect is known from other drugs with cationic amphiphilic properties. There is a possible relationship between this accumulation and the vacuolisation observed in lungs. This effect was only observed at high doses in rodents. The clinical relevance of these findings is unknown.
No genotoxicity has been observed following testing of memantine in standard assays. There was no evidence of any carcinogenicity in life long studies in mice and rats. Memantine was not teratogenic in rats and rabbits, even at maternally toxic doses, and no adverse effects of memantine were noted on fertility. In rats, foetal
growth reduction was noted at exposure levels, which are identical or slightly higher than at human exposure.
6 PHARMACEUTICAL PARTICULARS
6.1 List of excipients
Potassium Sorbate E202 Sorbitol E420 Purified water
6.2 Incompatibilities
Not Applicable
6.3 Shelf Life
36 months.
After first opening, the oral solution should be used within 12 weeks.
6.4 Special precautions for storage
This medicinal product does not require any special storage conditions.
If using the bottle with the mounted pump the bottle must be kept and transported in a vertical position.
6.5 Nature and contents of container
Amber glass bottles (Type III) containing either 50 ml, 100 ml or 10 x 50 ml solution with a screw cap(PP) and either a pump (PP and LDPE) or dosing pipette (LDPE and Polystyrol). The dosing pipette is printed in 0.5 ml graduations.
Not all packs may be marketed.
6.6 Special precautions for disposal
Any unused medicinal product or waste material should be disposed of in accordance with local requirements.
Instruction for proper use of Pump
Prior to first use the dosing pump has to be screwed on the bottle. For removing the screw cap from the bottle the cap must be turned anticlockwise ad unscrewed completely (fig.1).
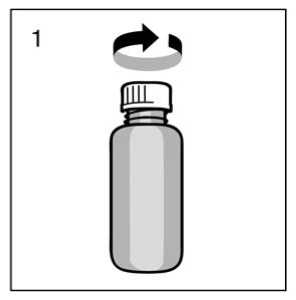
Mounting the dosing pump on the bottle:
The dosing pump has to be removed from the plastic bag (fig. 2) and placed on top of the bottle, sliding the plastic dip tube carefully into the bottle. Then the dosing pump needs to be held onto the neck of the bottle and screwed clockwise until it firmly attached (fig. 3). For the intended use the dosing pump is only screwed on once when starting the use, and should never be unscrewed.
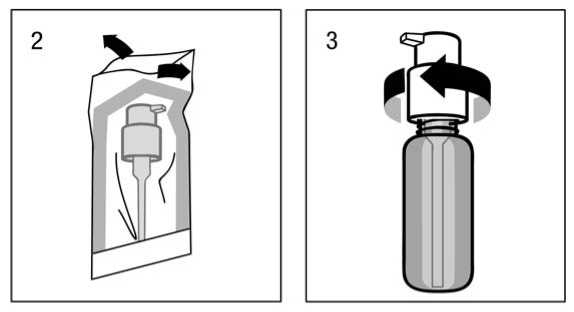
Use of the dosing pump for dispensing
The dosing pump head has two positions and is easy to turn -anticlockwise (unlocked position) and clockwise (locked position).The dosing pump head should not be pushed down while in the locked position. The solution may only be dispensed in the unlocked position. To do this, the dosing pump head has to be turned in the direction of the arrow about one eighth of a turn, until a resistance is felt fig. 4). The dosing pump is then ready for use.
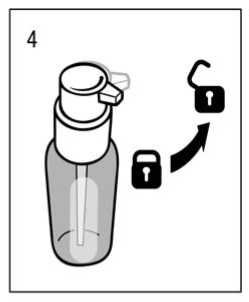
Preparing the dosing pump:
When used for the first time, the dosing pump does not dispense the correct amount of oral solution. Therefore, the pump must be prepared (primed) by pushing the dosing pump head down completely five times in succession (fig 5.)
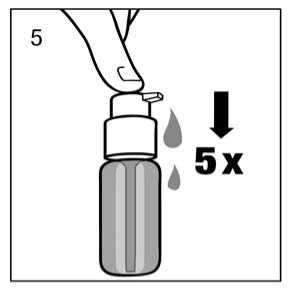
The solution thus dispensed is discarded. The next time the dosing pump head is pushed downwards completely (equivalent to one pump actuation), it dispenses the correct dose (1 pump actuation is equivalent to 0.5 ml oral solution, and contains 5 mg of the active substance memantine hydrochloride; fig 6.)
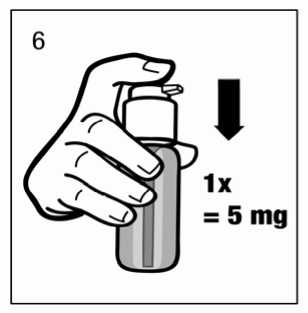
Correct use of the dosing pump:
A glass with a little water or a spoon should be held below the nozzle and the dosing pump head has to be pushed down in a firm but calm and steady manner (not too slowly) right down to the stop (fig. 7, fig. 8).
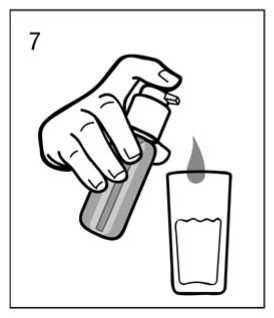
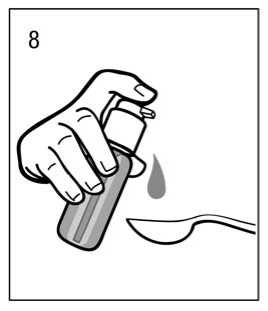
The dosing pump head can then be released and is then ready for the next pump compression.
The dosing pump may only be used with the <Invented Name> solution in the bottle provided, not for other substances or containers. If the pump does not function as described during intended use and according to instruction, the patient should consult the treating physician or a pharmacist. The dosing pump should be locked after use.
Instruction for proper use of Dosing Pipette Fig.1
Remove the cap from the bottle by turning it anti-clockwise.
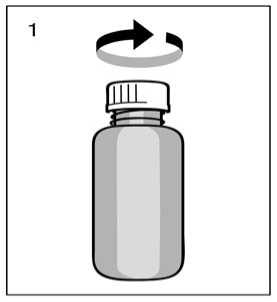
Fig.2
Insert the pipette into the bottle. While holding the bottom ring, pull the top ring up to the mark that corresponds to the number of millilitres or milligrams you need to give.
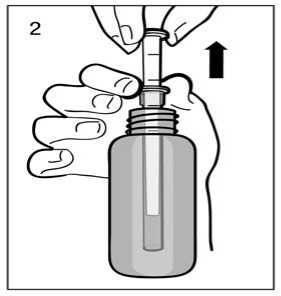
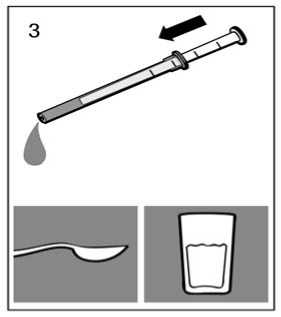
Fig.3
Holding the bottom ring, remove the entire pipette from the bottle.
The solution must not be pipetted into the mouth directly from the bottle but should be dosed onto a spoon or into a glass of water using the pipette.
7 MARKETING AUTHORISATION HOLDER
Torrent Pharma (UK) Ltd.
Unit 4, Charlwood Court,
County Oak Way Crawley
West Sussex. RH11 7XA United Kingdom
MARKETING AUTHORISATION NUMBER(S)
8
PL 36687/0117
9 DATE OF FIRST AUTHORISATION/RENEWAL OF THE AUTHORISATION
12/07/2013
10 DATE OF REVISION OF THE TEXT
15/10/2014