Aloflute 25 Microgram/250 Microgram Per Metered Dose Pressurised Inhalation Suspension
Package leaflet: Information for the user Aloflute
25 microgram/125 microgram per metered dose pressurised inhalation, suspension 25 microgram/250 microgram per metered dose pressurised inhalation, suspension
salmeterol/fluticasone propionate
Read all of this leaflet carefully before you start taking this medicine because it contains important information for you.
- Keep this leaflet. You may need to read it again.
- If you have any further questions, ask your doctor or pharmacist.
- This medicine has been prescribed for you only. Do not pass it on to others. It may harm them, even if their symptoms and signs of illness are the same as yours.
- If you get any side effects, talk to your doctor or pharmacist. This includes any possible side effects not listed in this leaflet. See section 4.
In this leaflet
1. What Aloflute is and what it is used for
2. What you need to know before you use Aloflute
3. How to use Aloflute
4. Possible side effects
5. How to store Aloflute
6. Contents of the pack and other information
1. What Aloflute is and what it is used for
Aloflute contains two medicines, salmeterol and fluticasone propionate.
• Salmeterol is a long-acting bronchodilator. Bronchodilators help the airways in the lungs to stay open. This makes it easier for air to get in and out. The effects last for at least 12 hours.
• Fluticasone propionate is a corticosteroid which reduces swelling and irritation in the lungs.
Aloflute is indicated for use in adults 18 years of age and older only.
Aloflute is NOT indicated for use in children 12 years of age and younger or adolescents 13 to 17 years of age.
The doctor has prescribed this medicine to help prevent breathing problems such as asthma.
You must use Aloflute every day as directed by your doctor. This will make sure that it works properly in controlling your asthma.
Aloflute helps to stop breathlessness and wheeziness coming on. However Aloflute should not be used to relieve a sudden attack of breathlessness or wheezing. If this happens you need to use a fast-acting ‘reliever’ (‘rescue’) inhaler, such as salbutamol. You should always have your fast-acting ‘rescue’ inhaler with you.
2. What you need to know before you use Aloflute Do not take Aloflute if:
Y ou are allergic (hypersensitive) to salmeterol, fluticasone propionate or any of the other ingredients of this medicine (listed in section 6).
Warnings and precautions
Your doctor will supervise your treatment more closely if you have medical conditions such as:
• Heart disease, including an irregular or fast heart beat
• Overactive thyroid gland
• High blood pressure
• Diabetes mellitus (Aloflute may increase your blood sugar)
• Low potassium in your blood
• Tuberculosis (TB) now, or in the past, or other lung infections
If you have ever had any of these conditions, tell your doctor before you use Aloflute.
Children and adolescents
This medicine should not be used in children or adolescents under the age of 18 years.
Other medicines and Aloflute
Tell your doctor or pharmacist if you are taking, have recently taken or might take any other medicines. This includes medicines for asthma or any medicines obtained without a prescription. This is because Aloflute may not be suitable to be taken with some other medicines.
Tell your doctor if you are taking the following medicines, before starting to use Aloflute:
• P blockers (such as atenolol, propranolol and sotalol). P blockers are mostly used for high blood pressure or other heart conditions.
• Medicines to treat infections (such as ritonavir, ketoconazole, itraconazole and erythromycin). Some of these medicines may increase the amount of fluticasone propionate or salmeterol in your body.
This can increase your risk of experiencing side effects with Aloflute, including irregular heart beats, or may make side effects worse.
• Corticosteroids (by mouth or by injection). If you have had these medicines recently, this might increase the risk of this medicine affecting your adrenal gland.
• Diuretics, also known as ‘water tablets’ used to treat high blood pressure.
• Other bronchodilators (such as salbutamol).
• Xanthine medicines. These are often used to treat asthma.
Pregnancy and breastfeeding
If you are pregnant or breastfeeding, think you may be pregnant or are planning to have a baby, ask your doctor or pharmacist for advice before taking this medicine.
Driving and using machines
Aloflute is not likely to affect your ability to drive or use machines.
3. How to use Aloflute
Always use this medicine exactly as your doctor or pharmacist has told you. Check with your doctor or pharmacist if you are not sure.
• Use Aloflute every day, until your doctor advises you to stop. Do not take more than the recommended dose. Check with your doctor or pharmacist if you are not sure.
• Do not stop taking Aloflute or reduce the dose of Aloflute without talking to your doctor first.
• Aloflute should be inhaled through the mouth into the lungs.
Adults aged 18 years and over
• Aloflute 25/125 - 2 puffs twice a day
• Aloflute 25/250 - 2 puffs twice a day
It is very important to follow your doctor’s instructions on how many puffs to take and how often to take your medicine.
If you are using Aloflute for asthma, your doctor will want to regularly check your symptoms. If your asthma or breathing gets worse tell your doctor straight away. You may find that you feel more wheezy, your chest feels tight more often or you may need to use more of your fast-acting ‘reliever’ medicine. If any of these happen, you should continue to take Aloflute but do not increase the number of puffs you take. Your chest condition may be getting worse and you could become seriously ill. See your doctor as you may need additional treatment.
Instructions for use
• Your doctor, nurse or pharmacist should show you how to use your inhaler. They should check how you use it from time to time. Not using Aloflute properly or as prescribed may mean that it will not help your asthma as it should.
• The medicine is contained in a pressurised canister in a plastic casing with a mouthpiece.
• There is a counter on the back of the inhaler which tells you how many doses are left. Each time you press the canister, a puff of medicine is released and the counter will count down by one.
• Take care not to drop the inhaler as this may cause the counter to count down.
Testing your inhaler
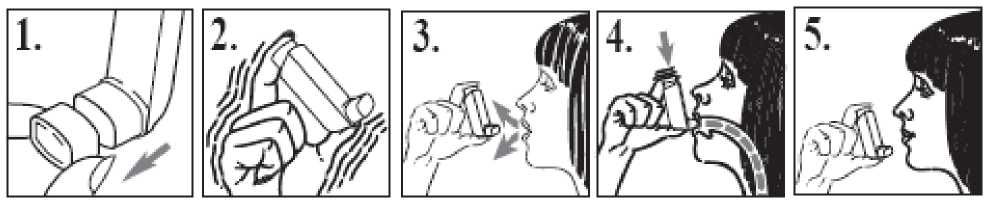
1. When using your inhaler for the first time, test that it is working. Remove the mouthpiece cover by gently squeezing the sides with your thumb and forefinger and pull apart (figure 1).
2. To make sure that the inhaler works, shake it well, point the mouthpiece away from you and press the canister firmly to release a puff into the air. Repeat these steps at least three times, shaking the inhaler before releasing each puff, until the counter reads 120. If you have not used your inhaler for a week or more, or your inhaler gets very cold (below 0°C) you should release two puffs of medicine into the air.
Using your inhaler
It is important to start to breathe as slowly as possible just before using your inhaler.
1. Stand up or sit upright when using your inhaler.
2. Remove the mouthpiece cover (figure 1). Check inside and outside to make sure that the mouthpiece is clean and free of loose objects.
3. Shake the inhaler 4 or 5 times to ensure that any loose objects are removed and that the contents of the inhaler are evenly mixed (figure 2).
4. Hold the inhaler upright with your thumb on the base, below the mouthpiece. Breathe out as far as is comfortable (figure 3).
5. Place the mouthpiece in your mouth between your teeth. Close your lips around it. Do not bite.
6. Breathe in through your mouth slowly and deeply. Just after starting to breathe in, press firmly down on the top of the canister to release a puff of medicine. Do this while still breathing in steadily and deeply (figure 4).
7. Hold your breath, take the inhaler from your mouth and your finger from the top of the inhaler. Continue holding your breath for a few seconds, or as long as is comfortable (figure 5).
8. Wait about half a minute between taking each puff of medicine and then repeat steps 3 to 7.
9. Afterwards, rinse your mouth with water and spit it out, and/or brush your teeth. This may help to stop you getting thrush and becoming hoarse.
10. After use always replace the mouthpiece cover straight away to keep out dust. The mouthpiece cover will ‘click’ into position. Do not use too much force.
Do not rush steps 4, 5, 6 and 7. It is important that you breathe in as slowly as possible just before using your inhaler. You should use your inhaler whilst standing in front of a mirror for the first few times. If you see "mist" coming from the top of your inhaler or the sides of your mouth, you should start again from step
3.
If you find it difficult to use your inhaler, either your doctor or other healthcare provider may recommend using a spacer device such as the AeroChamber Plus® with your inhaler. Your doctor, nurse, pharmacist or other healthcare provider should show you how to use the spacer device with your inhaler and how to care for your spacer device and will answer any questions you may have. It is important that if you are using a spacer device with your inhaler that you do not stop using it without talking to your doctor or nurse first. Only the AeroChamber Plus® spacer device should be used with Aloflute. Other spacing devices should not be used with Aloflute and you should not switch from one spacer device to another. If you stop using a spacer device your doctor may need to change the dose of medicine required to control your asthma. Always talk to your doctor before making any changes to your asthma treatment.
People with weak hands may find it easier to hold the inhaler with both hands. Put the two forefingers on top of the inhaler and both thumbs on the bottom below the mouthpiece.
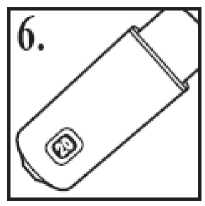
You should get a replacement when the counter shows the number 20 (figure 6). Stop using the inhaler when the counter shows 0 as any puffs left in the device may not be enough to give you a full dose. Never try to alter the numbers on the counter or detach the counter from the plastic casing.
Cleaning your inhaler
To stop your inhaler blocking, it is important to clean your inhaler at least once a week.
To clean your inhaler
• Remove the mouthpiece cover.
• Do not remove the canister from the plastic casing at any time.
• Wipe the inside and outside of the mouthpiece and the plastic casing with a dry cloth or tissue.
• Replace the mouthpiece cover. It will ‘click’ into place. Do not use too much force.
Do not wash or put any parts of your inhaler in water.
If you use more Aloflute than you should
It is important to use the inhaler as instructed. If you accidentally take a larger dose than recommended, talk to your doctor or pharmacist. You may notice your heart beating faster than usual and that you feel shaky. You may also have dizziness, a headache, muscle weakness and aching joints.
If you have used larger doses for a long period of time, you should talk to your doctor or pharmacist for advice. This is because larger doses of Aloflute may reduce the amount of steroid hormones produced by the adrenal gland.
If you forget to use Aloflute
Do not take a double dose to make up for a missed dose. Just take your next dose at the usual time.
If you stop using Aloflute
It is very important that you take your Aloflute every day as directed. Keep taking it until your doctor tells you to stop. Do not stop or suddenly reduce your dose of Aloflute. This could make your breathing worse.
In addition, if you suddenly stop taking Aloflute or reduce your dose of Aloflute this may (very rarely) cause you to have problems with your adrenal gland (adrenal insufficiency) which sometimes causes side effects.
These side effects may include any of the following:
• Stomach pain
• Tiredness and loss of appetite, feeling sick
• Sickness and diarrhoea
• Weight loss
• Headache or drowsiness
• Low levels of sugar in your blood
• Low blood pressure and seizures (fits)
When your body is under stress such as from fever, trauma (such as a car accident), infection, or surgery,
adrenal insufficiency can get worse and you may have any of the side effects listed above.
If you get any side effects, talk to your doctor or pharmacist. To prevent these symptoms occurring, your doctor may prescribe extra corticosteroids in tablet form (such as prednisolone).
If you have any further questions about the use of this medicine, ask your doctor, nurse or pharmacist.
4. Possible side effects
Like all medicines, this medicine can cause side effects, although not everybody gets them. To reduce the chance of side effects, your doctor will prescribe the lowest dose of Aloflute to control your asthma.
Allergic reactions: you may notice your breathing suddenly gets worse immediately after using Aloflute. You may be very wheezy and cough or be short of breath. You may also notice itching, a rash (hives) and swelling (usually of the face, lips, tongue, or throat), or you may suddenly feel that your heart is beating very fast or you feel faint and light headed (which may lead to collapse or loss of consciousness). If you get any of these effects or if they happen suddenly after using Aloflute, stop using Aloflute and tell your doctor straight away. Allergic reactions to Aloflute are uncommon (they affect less than 1 person in 100).
Other side effects are listed below:
Very Common (affects more than 1 person in 10)
• Headache - this usually gets better as treatment continues.
Increased number of colds have been reported in patients with chronic obstructive pulmonary disease (COPD).
COPD is a long-term lung disease that causes shortness of breath, coughing and frequent chest infections. The term COPD includes conditions known as chronic bronchitis and emphysema.
Common (affects less than 1 person in 10)
• Thrush (sore, creamy-yellow, raised patches) in the mouth and throat. Also sore tongue and hoarse voice and throat irritation. Rinsing your mouth out with water and spitting it out immediately and/or brushing your teeth after taking each dose of your medicine may help. Your doctor may prescribe an anti-fungal medication to treat the thrush.
Aching, swollen joints and muscle pain.
• Muscle cramps.
The following side effects have also been reported in patients with COPD:
• Pneumonia and bronchitis (lung infection). Tell your doctor if you notice any of the following symptoms: increase in sputum production, change in sputum colour, fever, chills, increased cough, increased breathing problems.
• Throat irritation. Rinsing your mouth out with water and spitting it out immediately after taking each puff may help.
• Bruising and fractures.
• Inflammation of sinuses (a feeling of tension or fullness in the nose, cheeks and behind the eyes, sometimes with a throbbing ache).
• A reduction in the amount of potassium in the blood (you may get an uneven heart beat, muscle weakness, cramp).
Uncommon (affects less than 1 person in 100)
• Increases in the amount of sugar (glucose) in your blood (hyperglycaemia). If you have diabetes, more frequent blood sugar monitoring and possibly adjustment of your usual diabetic treatment may be required.
• Cataract (cloudy lens in the eye).
• Very fast heart beat (tachycardia), or a rapid and irregular heartbeat (atrial fibrillation).
• Feeling shaky (tremor) and fast or uneven heart beat (palpitations) - these are usually harmless and get less as treatment continues.
• Chest pain.
• Feeling worried (this effect mainly occurs in children).
• Disturbed sleep.
• Allergic skin rash.
Rare (affects less than 1 person in 1000)
• Breathing difficulties or wheezing that get worse straight after taking Aloflute. If this happens stop using your Aloflute inhaler. Use your fast-acting “reliever” inhaler to help your breathing and tell your doctor straight away.
• Aloflute may affect the normal production of steroid hormones in the body, particularly if you have taken high doses for long periods of time. The effects include:
- Slowing of growth in children and adolescents
- Thinning of the bones
- Glaucoma
- Weight gain
- Rounded (moon shaped) face (Cushing’s Syndrome)
Your doctor will check you regularly for any of these side effects and make sure you are taking the lowest dose of Aloflute to control your asthma.
• Behavioural changes, such as being unusually active and irritable (these effects mainly occur in children).
• Uneven heart beat or heart gives an extra beat (arrhythmias). Tell your doctor, but do not stop taking Aloflute unless the doctor tells you to stop.
• A fungal infection in the oesophagus (gullet), which might cause difficulties in swallowing. Frequency not known, but may also occur:
• Depression or aggression. These effects are more likely to occur in children.
Reporting of side effects
If you get any side effects, talk to your doctor or pharmacist. This includes any possible side effects not listed in this leaflet.
You can also report side effects directly via the Yellow Card Scheme at: www.mhra.gov.uk/yellowcard.
By reporting side effects you can help provide more information on the safety of this medicine.
5. How to store Aloflute
• Keep this medicine out of the sight and reach of children.
• Do not use Aloflute after the expiry date which is stated on the label and carton after EXP. The expiry date refers to the last day of that month.
• Do not store above 25°C.
• The canister contains a pressurised liquid. Do not expose to temperatures higher than 50°C, protect from direct sunlight. Do not pierce or burn the canister even when empty.
• As with most inhaled medicinal products in pressurised canisters, the therapeutic effect of this medicinal product may decrease when the canister is cold.
Do not throw away medicines via wastewater or household waste. Ask your pharmacist how to throw away
medicines you no longer use. These measures will help protect the environment.
6. Contents of the pack and other information What Aloflute contains
• Each metered dose (ex valve) contains 25 micrograms of salmeterol (as salmeterol xinafoate) and 125 or 250 micrograms of fluticasone propionate. This is equivalent to a delivered dose (ex actuator) of 21 micrograms of salmeterol and 110 or 220 micrograms of fluticasone propionate. The other ingredients are the propellant, norflurane (HFA 134a) and ethanol, anhydrous.
What Aloflute looks like and contents of the pack
• Aloflute is supplied to you in a metered dose inhaler which delivers your medicine in a pressurised suspension for you to inhale through your mouth into your lungs.
• The pressurised canister contains a white to off white suspension for inhalation.
• The canisters are fitted into a white plastic casing incorporating a mouthpiece and fitted with mauve or burgundy dustcaps.
• The devices are packed in cartons of 1 inhaler. Each inhaler contains 120 metered doses.
Marketing Authorisation Holder and Manufacturer
Marketing Authorisation Holder:
3M Health Care Ltd 3M House 1 Morley Street Loughborough LE11 1EP UK
Manufacturer:
3M Health Care Ltd Derby Road Loughborough Leicestershire LE11 5SF UK
This leaflet was last revised 04/2015
AeroChamber Plus is a trademark of Trudell Medical International 3M is a trademark of 3M Company © 3M Company 2015
8